We digest and absorb nearly 97% of the food we consume. However, our absorptive ability is severely restricted when the lining of our intestines becomes irritated or flattened. This can occur with food allergies, food intolerances and/or inflammatory bowel diseases. If these issues aren’t resolved, nutrient absorption will not occur.
What is a food allergy?
The immune system is a group of cells that help to protect our body from infectious agents. An allergic reaction to food involves an immune system response that starts with a protein molecule made by the body, called an antibody, which helps battle viruses and bacteria. An antibody can connect with and attach to a specific target, known as its antigen, which is usually located on the virus, bacterium, or allergen. Once bound to the invader, it’s like a red alert, calling out the invading allergen, and provoking the body’s immune system to attack it.
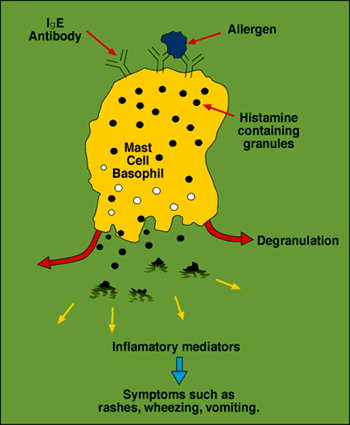
The main antibody in most allergic conditions is called immunoglobulin E (IgE). With a food allergy, IgE antibodies are produced in response to an innocent food molecule. IgE antibodies are found on the surface of mast cells, and when activated, trigger the mast cells to release various chemical messengers.
Millions of mast cells line our skin, nose, intestines, and bronchial tubes. In a normal immune response, the IgE/mast cell combo means bad news for microbes. In an exaggerated response, such as with an innocent food molecule, we have the symptoms that come with a severe food allergy. In both cases, these symptoms typically occur in the areas that have a lot of mast cells: skin, nasal passages and airway, and gastrointestinal tract.
Think of the mast cell like one of those loud, obnoxious car alarms. It doesn’t always go off due to a true car thief (car thief = virus, bacteria, and/or parasite). It may be triggered by a strong wind or a passing jogger (the innocent food molecule).
A cascade of events occur when chemical messengers are released from mast cells, including dilated blood vessels, a drop in blood pressure, and swelling of the lips, mouth, tongue and throat. This combination of symptoms, when powerful enough, is referred to as anaphylaxis. A common example of this is a peanut or shellfish allergy. If someone eats one of these foods and has a true allergy, they could die without medical assistance. It’s a severe condition with severe consequences.
Food allergens can come into the body by one route, but cause symptoms somewhere else entirely because they travel in the bloodstream. Since this connection between food and symptoms isn’t always obvious, proving immune system involvement with a particular food usually requires a positive skin-prick test. A laboratory test measure of IgE response can confirm a food allergy as well. However, not all food allergies involve IgE.
It’s estimated that 3-7% of children and about 2% of adults suffer from food allergy.
The 8 most common food allergens
- Milk
- Eggs
- Peanuts
- Tree nuts (e.g., almonds, cashews, walnuts)
- Fish
- Shellfish
- Soy
- Wheat
What is a food intolerance?
Many people say they are “allergic” to foods when they are actually intolerant. Food intolerances usually occur when the gut reacts poorly to a specific food or ingredient used in food preparation. Intolerances can result from the absence of an enzyme needed to fully digest a food, such as with lactose intolerance.
Food intolerance is not regarded as a sound diagnosis by much of the medical community. In part, this may be because symptoms of food intolerance are milder and usually have a slower onset than food allergy (but not always). These symptoms can include gas/bloating, diarrhea, stomach cramping, stuffy nose, mucus production, nausea, vomiting, headaches, etc. While some of these symptoms are benign, serious gastrointestinal complaints are often characteristic of severe intolerance; if left uninvestigated, more serious problems can result.
Common culprits in food intolerance tend to be foods eaten very regularly, like wheat, milk, corn, and more recently, soy. Lactose intolerance is a common example. In people without enough lactase enzyme activity, undigested lactose from dairy products passes through the stomach into the intestines, where it must be fermented. Through this process, lots of gas is formed, causing stomach cramps, bloating, flatulence, and diarrhea. Compounding the problem, other symptoms can be a result of milk protein sensitivity. While casein protein has been implicated in more cases of milk protein problems than whey, both milk proteins can cause similar issues. This is because both casein and whey can cause an excessive inflammatory response in some individuals, leading to mucus production. High mucus means blocked airways, stuffy noses, and thick throats. Unlike an allergy, in which sensitive people can react to minute quantities (or even odours), a food intolerance usually requires a larger quantity of food to be consumed before symptoms arise.
Intolerances are much more prevalent than food allergies; however, because the symptoms are milder and often not immediate, people can be unsure which foods are causing the problem. Thus, food intolerance testing is becoming more frequent. Eliminating and re-introducing the suspected food in the diet is a dependable way to assess food intolerance.
The most common food intolerances are:
| Type | Found in |
| Lactose or milk protein | Dairy (esp. cow’s milk) |
| Yeast (Candida albicans) | Breads and baked goods; can be exacerbated by sugar |
| Gluten (including both celiac and wheat sensitivity) | Grains such as wheat, barley, and rye |
| Fructose | Fruit; foods sweetened with fructose (as well as sorbitol) |
Others may include:
| Type | Found in |
| Food additives | Processed foods |
| Amines | Fermented foods, e.g. sauerkraut, pickles, cheeses |
| Salicylates | Fruits (such as apples, avocados, blueberries, dates, kiwi fruit, peaches, raspberries, figs, grapes, plums, strawberries, cherries, grapefruit and prunes); Vegetables (such as alfalfa, cauliflower, cucumbers, mushrooms, radishes, broad beans, eggplant, spinach, zucchini, broccoli and hot peppers); Some cheeses; Herbs, spices, and condiments (such as dry spices and powders, tomato pastes and sauces, vinegar, and soy sauce, jams and jellies); Beverages (such as coffee, wine, beer, orange juice, apple cider, regular and herbal tea, rum and sherry); Some nuts; Mint; Artificial flavourings |
| Nitrates | Processed foods, e.g. preserved meats |
| Monosodium glutamate | Processed foods |
| Propionates | A preservative in commercial breads |
| Some antioxidants | Processed foods (used to prevent spoilage) |
It’s been estimated that 3 in 4 people have some form of food intolerance, whether mild or severe. And these intolerances are uniquely individual. Everything from the nutrients and chemicals above, to specific minerals, to specific food additives can lead to a host of symptoms. Note that eating the PN way, i.e. a diet that is low in processed foods, can help eliminate many of these common food offenders.
Another common type of food intolerance is Leaky Gut Syndrome (LGS). LGS is poorly recognized, and rarely tested for, but fairly common. With LGS, the intestinal lining becomes extremely permeable, meaning that it may allow large molecules and toxins to enter the body undigested. This is possible when the intestinal lining becomes inflamed or damaged, disrupting its normal functions. As a result, “spaces” develop between the cell walls and macromolecules (including histamine from food), antigens, and toxins sneak in. As these molecules, which should not be allowed to sneak in, invade the GI wall more frequently, additional damage occurs, exacerbating the problem.
Beyond damaging the intestinal mucosa, these molecules (which are much larger than the body prefers to absorb) can be treated as foreign invaders that trigger the body’s immune defenses. This sets off a cascade of antibody production. The body sets up a defense against otherwise healthy food, and potentially against its own cells, although this is speculative. To make matters worse, as the damage to the intestinal mucosa gets worse, the carrier proteins also become damaged, causing nutrient deficiency. There are many symptoms of LGS including GI distress (bloating, flatulence, and abdominal discomfort), immune reactions (including hives and mucus build up), nutrient deficiency, and more. The symptoms of LGS are similar to those of food intolerances.

Other interesting information about food sensitivities
Food allergies are usually present for years, or even a lifetime. Food intolerances can dissipate after several months, only recurring if the food is eaten regularly again.
Human beings do a fairly poor job at identifying foods that cause non-acute, long-term illness. It took a famine in Holland at the end of World War II to eradicate wheat from the diet, and an attentive doctor to identify that his celiac patients had been cured.
Some foods contain large amounts of histamine, the same inflammatory mediator released by mast cells. This can cause unpleasant symptoms, such as those listed above along with neuropathic symptoms (tingling, pins and needles), flushing of the skin, racing heart and other symptoms of anxiety and agitation (perhaps what scientists might refer to technically as “ants in your pants”). Well ripened cheeses and sausages are the main offenders, along with some types of fish, sauerkraut and alcoholic drinks. The liver can metabolize histamine, however, the drug isoniazid (for treating tuberculosis) can limit the ability of the liver to break down histamine. Thus, anyone on isoniazid should avoid foods with histamine.
Infants delivered via Cesarean section may have an increased risk of developing food allergies. The low compressive forces against the infant during a Cesarean delivery might delay the growth of normal intestinal flora.
Among all allergic reactions, food allergy is the leading cause for emergency room visits in the United States, Great Britain, Canada, France and Australia.
Summary & recommendations
If you suspect you may have a food sensitivity, it’s important to first rule out the possibility of a true food allergy. This can be done with your physician. If you suspect you may have a food intolerance, keeping a diligent food diary/response log can help find the offending foods quickly and remove them.
Because of the delay between food ingestion and response, it’s easy to ignore food intolerance symptoms or simply accept them as part of life. If any of the symptoms listed in this article are part of your normal day, you might look at your food intake to see what might be causing the problem(s).
Measures that may prevent food sensitivities
- Varying the diet
- Avoiding high quantities of high risk foods
- Getting breast fed for the first year of life
- Limiting excessive amounts of caffeine
- Avoiding compounds that increase gut permeability, such as alcohol, spicy foods, raw pineapple, raw papaya, aspirin and other NSAIDs
- Limiting exposure to pesticides, herbicides and fungicides used on food crops
Further resources
Food Allergy & Anaphylaxis Network
Gluten intolerance and celiac disease
Lactose intolerance and milk/casein allergy
Fructose intolerance/malabsorption
References
Click here to view the information sources referenced in this article.
Eat, move, and live… better.©
Yep, we know… the health and fitness world can sometimes be a confusing place. But it doesn’t have to be.
Let us help you make sense of it all with this free special report.
In it you’ll learn the best eating, exercise, and lifestyle strategies — unique and personal — for you.



Share