Many behaviours qualify as addictions — things we feel overwhelmingly compelled to do, despite the consequences. What’s food addiction, and how can we treat it?
When asked what substance he was first addicted to, guitarist Eric Clapton answered: “sugar.” And we all know the person who kicked the “hard drugs” only to become reliant on food as their “go-to” addiction of choice.
So, are we all doomed for food addiction?
Well, 97% of people prescribed opioid painkillers (with no history of addiction) don’t become addicts. And most of us wouldn’t rob a 7-11 for candy bars if the price of candy bars became unaffordable. But some people are more susceptible to addiction, whether it’s opioids or candy bars.
Thus, addiction is complicated: Social, motivational, emotional, and genetic factors all interact to create an addiction experience. An addictive substance alone doesn’t create addiction. However, some things are more addictive than others.
We often joke “I’m a ___ addict”, whether that’s video games, shoes, or ice cream. But what, exactly, is real addiction? And is it a useful concept for understanding food behaviour?
What is addiction?
Addiction is an overpowering craving to repeatedly engage in an activity that provides temporary relief at the expense of terrible consequences. It’s something you feel compelled to do, even though it harms you.
To count as an addiction, there must also be withdrawal — feelings of discomfort, distress, and intense cravings — when our addictive substance or behaviour is taken away or stopped.
What is food addiction?
Thus, food addiction involves a regular compulsion to eat and/or consume particular foods, even though those foods harm us — whether that’s because the foods are unhealthy (e.g. high in sugar), or because they make us sick, or cause us to become obese.
An occasional big meal: not addiction. Regularly eating so much, and so rapidly, that you end up bloated and nauseated — but feel unable to stop? Potential addiction.
After having a couple of cookies (or any potentially addictive food), a non-addict will feel indifferent about eating more. The experience of an addict is much different. Addicts become utterly single-minded in the pursuit of their “hit”. Eating a couple of cookies (or any potentially addictive food) sets off an abnormal reaction – and they want more and more until they’re physically unable to swallow.
If you aren’t an addict, it’s not that you are a master of self-control, you just don’t have an insatiable appetite for more.
A food addict can be:
- an overweight woman who is always trying a new diet
- a man who eats beyond fullness at dinner after snacking on junk food all day to help deal with job stress
- a thin woman who never eats enough and is hungry all the time because she’s afraid of getting fat (in this case, her “hit” is not eating)
- a lonely guy with nothing to do on a Friday night except watch TV and eat several bags of chips
- a person who snacks all day to ease the boredom of an un-stimulating life
- a perfectionist who is never quite satisfied with their body
- a person suffering from a nutrition related disease (e.g., heart disease, diabetes, etc.) who gets disturbingly resistant when presented with treatment approaches
Some food addicts eat too much; some don’t consume enough. For a food addict, food provides the fun, entertainment, control, reassurance, or love that’s missing in their life. Food may also help to numb difficult emotions like fear and sadness. Some people even have addiction to restriction.
The Yale Food Addiction test is a clinical tool for assessing food addiction (click to download in PDF).
Food dependence
But here’s the problem with determining food addiction: Unlike, say, heroin or gambling, we need food to live. Without an innate desire for food, we can wave bye-bye to evolution.
At what point does “big appetite” end and “food addiction” begin? And can you technically become “addicted” to something you need?
Researchers, while divided on the exact definition of “food addiction” or whether it truly exists, nevertheless agree that addiction is a pattern of behaviour characterized by things like:
- near-constant searches for a “hit”
- an intense compulsion and/or desire for the substance or behaviour
- strong, all-encompassing focus on getting that “hit”
- withdrawal symptoms when the “hit” is taken away
- needing more, or more intense “hits” as tolerance develops over time
By this definition, nearly anything — including food, water, or sex (i.e. things that are part of basic biology) — can be an addiction.
So let’s call it “food dependence”.
Over time, food (substance) dependence often becomes less about the high and more about preventing the negative feelings that come from abstinence. The ability to get pleasure from the food becomes more difficult, because small amounts of the same food aren’t as rewarding.
Substance dependence: Official definitions
The Diagnostic and Statistical Manual of Mental Disorders (DSM-IV) defines “substance dependence” as 3 or more of the following 7 symptoms occurring within 1 year. We’ll look at how these might relate to food dependence.
Symptom 1: I use more over time.
Over time, tolerance increases.
Food example: When I used to buy groceries, I would take them home, eat a snack and go on with my day. Now I buy groceries and I eat all day long until I have gone through half of what I bought.
Symptom 2: I have withdrawal symptoms.
I now take the substance to avoid withdrawal.
Food example: I eat processed snacks to correct being tired and/or depressed. To fix anxiety, I eat something crunchy, like chips or crackers to calm myself. I am afraid if I stop using food to correct my emotions, I will have nothing else to turn to.
Symptom 3: I use more than I intend.
Food example: One bowl of ice cream turns into 2 bowls, then 3 bowls. I start with one handful of chips and end up eating the whole bag.
Symptom 4: I’m trying or have tried to cut back.
I want to reduce my intake, and I’ve tried, but haven’t been successful.
Food example: I have tried to cut down or stop my eating, but it’s always on my mind and I find a way to defeat myself, even making a special trip to get a candy bar or chips.
Symptom 5: I spend time pursuing, using, or recovering from use.
I spend a lot of time on activities necessary to obtain the substance, or recover from its effects.
Food example: I will have a list of chores to do on Saturday. I will go to the store and buy groceries and spend the rest of the day eating what I bought, taking antacids, and sleeping.
Symptom 6: I miss important activities because of my substance use.
I miss or give up important social, occupational, or recreational activities.
Food example: I come home and eat. Then, I’m too full to exercise or meet with friends.
Symptom 7: I eat despite knowing the consequences.
I continue to abuse the substance despite knowing it’s giving me a persistent or recurrent physical or physiological problem.
Food example: I eat in spite of horrible knee pain from obesity. I’m so uncomfortable after a binge that I can’t lay down without regurgitation into my esophagus. My blood pressure is high. I’m miserable. I am embarrassed and afraid about being in social situations but I overeat anyway.
What influences food addiction?
Many factors play a role in the development of food addiction.
Fear: Addicts may fear eating a reasonable amount of food, getting fat, and/or experiencing uncomfortable emotions and hunger.
Chronic overeating: Eating too much of highly processed foods can stimulate brain opiates — “feel good” chemicals. Regular bingeing might create a dependency on this “natural high”. We become dependent on a highly processed diet to feel “normal” and experience withdrawal symptoms when we don’t eat it.
Food restriction: What if I told you that starting tomorrow you could never have ice cream again? What would you do today? Probably eat a bunch of ice cream – right? Cravings and reward responses from food are greater after a period of food restriction (whether real or imagined) and/or nutrient depletion. This is why diets and extreme restriction almost inevitably lead to binges.
Stress: Various forms of stress can trigger addiction. Binging + food restriction + stress = a winning combination for food addiction. Addiction can lie dormant when things are going well, then rear its ugly head when life trouble strikes.
Depression: Depression usually changes appetite, hunger, and fullness signals, as well as sleep patterns (normally, good quality sleep helps us manage urges — sleep is “willpower fuel”).
Weak satiety mechanisms: Some people who struggle with food addiction aren’t as tuned in to their fullness cues. They “hear” hunger signals more loudly than satiety signals.
Automaticity: Food behaviours can be strongly ingrained habits that “wear a groove” into our nervous system. Some argue that they can’t be eliminated — just rendered dormant (temporarily).
What makes food addictive?
Are all pleasurable foods automatically addictive? Probably not.
Hyperpalatability
Processed foods are engineered in ways that exceed basic reward properties of traditional whole foods, making them hyperpalatable.
Consider items such as ice cream, burgers, candy, melted cheeses, buttery/oily sauces, and so on – these are the foods that stimulate the release of opioids and dopamine in the brain and have addictive potential (note: artificial sweeteners can even trigger a dopamine response).
Rodent studies confirm this: Rats are unlikely to binge on normal rat chow. But when given the option of sweeter and fattier rat chow, rats go on a bender.
The table below shows the characteristics of some “normal” foods and some hyperpalatable foods. Notice how much higher in sugar, fat, and/or sodium the hyperpalatable foods are — and how many ingredients each food contains.
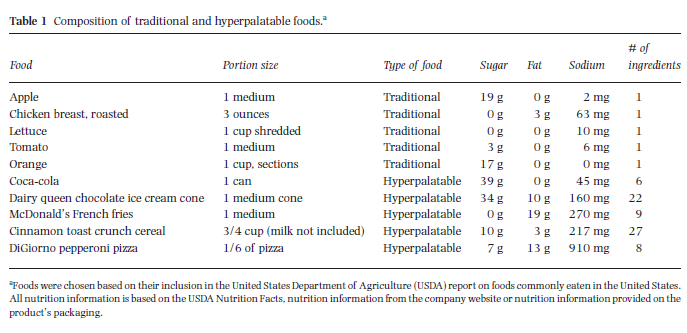
Other things can contribute to the addictive potential of food:
Quantity: When served more, we eat more.
Processing & energy density: The right mix of fat, sweeteners, flours, caffeine and salt provides a strong reward. Plain sugar packets or a bottle of olive oil aren’t very desirable. Processed foods have combinations of ingredients not found in nature. Many food components, like drugs, are not addictive until extracted and concentrated by modern processing (a whole grain vs. white flour in cake, a whole fruit vs. sugar in cookies, cocaine vs. cocoa leaves, opium vs. poppies, etc.).
Variety: When there are different colours, sizes, shapes, tastes, and textures, we eat more. People will eat more cookie dough ice cream versus plain vanilla and more trail mix versus plain raw almonds.
Nutrient composition of foods: When we eat nutrient-poor foods, we may end up eating more overall food in order to meet nutrient needs.
Access: The number one factor in addiction is availability. If the substance isn’t available, we can’t develop an addiction. When the substance is readily available, addiction will be more common (think: cigarettes in vending machines).
Cultural norms: When a behavior/substance is accepted within a group, it’s unlikely that behaviour will stop. Many folks cut down on or quit smoking when jurisdictions outlawed smoking in restaurants and bars.
Individual preferences
Think about what foods have an “addictive” potential for you. It’s important to consider these questions because any one food isn’t universally “addictive.”
- What foods do you crave?
- What foods do you think about you aren’t physically hungry?
- What foods do you want to eat more of, even when you’re full?
- What foods do you typically deprive yourself of — but later, feel unable to control yourself around?
- What foods have emotional associations for you — say, foods you remember from childhood, or foods that seem to have “special powers” to make you feel better?
Answers to the aforementioned questions don’t usually include barley, pears, asparagus and black beans (but it’s possible).
While whole foods in their most unprocessed form are still potentially addictive (think sweet fruits and fatty nuts), the potential for true dependence/addiction is low compared to processed foods (such as fruit candies and flavoured fatty nuts).
Treating addiction
People aren’t responsible for having an addiction, but they are responsible for dealing with it.
To treat addiction, you must address the following factors:
Food availability and environment
If you feel out of control with certain foods or in certain situations, you probably are.
Our behaviour depends heavily on social and environmental cues. We can adjust our behaviour by adjusting cues from our routine and environment.
Thus: Avoid people, places, and things that trigger addiction. Use social pressure to your advantage. Addicts don’t like to use their drug with sober people staring at them.
The more available — and socially acceptable — an addictive substance is, the easier it is to get hooked. Make it hard to get.
Emotions
Food doesn’t help resolve emotions. And emotions aren’t a bad thing. They actually serve a useful purpose in life and can indicate that something is out of balance.
Food can be used as a coping mechanism for emotions that feel intolerable. Once a “food rush” wears off, we’re left with the very same emotional problems… plus the additional problems addiction brings.
Many addictions stem from uncontrolled stress combined with food restriction. If these two factors can be controlled, food addiction might also be controlled.
Pharmaceuticals
What about appetite suppressants and drugs that eliminate the high from addictive foods? These so-called solutions open up new problems (e.g., undereating, malnutrition, etc).
Compliance to pharmaceuticals like naltrexone (blocks the high someone gets from a drug) and antabuse (makes someone sick if they drink alcohol) tend to be poor. Why? Because people want the high again. Even if an appetite suppressant drug is developed, the food addiction will still remain. This has little to do with the addictive food itself and more to do with a deficiency elsewhere in life – boredom, loneliness, anger, lack of stimulation, lack of purpose, etc.
Cravings die as a side effect of changing our life and identity — medication is, at best, only a partial and temporary solution.
However, pharmaceuticals that may be useful in addiction recovery include those that treat underlying conditions leading to emotional distress (pain, depression, etc.).
Abstinence
While we can’t choose to be addicted, we can choose to abstain in order to sustain recovery. Some claim that as an addict, it’s easier to give up the addictive substance entirely than to negotiate with it.
In this case, freedom comes when we give up effort to control the substance and become abstinent. Recovery from addiction means having the restoration of choice.
However, abstinence means that addicts must be willing to face discomfort. Luckily, the longer an addict remains abstinent, the more biological urges for the substance fade. Withdrawal is worst in the beginning.
If urges return, they’re often the result of conditioned reflexes and/or the desire to escape emotional distress. Managing stress and knowing “triggers” is thus an important part of recovery.
Meaning
Recovery from addiction needs meaning and purpose. Without meaning, there is no reason to remain abstinent.
External meanings (e.g., how the body looks, a spouse, a friend) can be fleeting. We love them one day, hate them the next.
If we count on external meanings for sustained change, there’s a good chance we’ll be dissatisfied. Dissatisfaction fuels resentment, and soon enough we remember that overeating is a quick way to forget about the entire mess.
Meaning is one of the reasons why the idea of a “higher power” in many addiction recovery programs is appealing. A higher power isn’t fleeting, it’s eternal. However, what’s most important is that the meaning and purpose is internal — it comes from the inside and reflects the person’s deeper values and life priorities.
Getting a handle on food addiction often requires a temporary hiatus from mirror and scale obsession. Instead, we must prioritize what’s going on inside.
Dieting
Reason is no match for addiction. Addiction is mostly an emotional-biological phenomenon.
Thus, addicts tend to be unable to rely on self-control alone — which doesn’t mean they are “weak”. (In fact, given how hard most food addicts try to change — even if unsuccessfully — arguably their will is very strong.)
The struggle with food addiction often leads to dieting, over-exercising, purging, drugs, binging, and weight gain/loss. These are efforts to control the addiction, but these efforts are often unrealistic, become lenient, and eventually fail (and this failure can lead to more addictive behaviors). In fact, restriction and obsession with “fixing the problem” itself can create more rebounds.
Structural changes
“Willpower” helps, but it’s weak compared to structural and foundational changes. This includes things like:
- changing one’s physical environment
- building a social support system (including getting away from people who enable the addiction)
- making it tougher to get at the addictive substances
- decreasing life stress, and/or working on stress management
- learning to tolerate discomfort, and getting support in doing so
- changing one’s routine and schedule to favour positive behaviours, and diminish the chances for negative behaviours (which can include things like getting more sleep, seeking out safer situations during “trigger times”, scheduling activities that conflict with the addictive behaviour, etc.)
Other tidbits and factoids
Food addiction factoids
Reward threshold — or the amount of substance needed to get a “high” — increases over time. Addicts need more and more. Eventually, many don’t get a “high” or any pleasure at all — the addiction focuses around managing withdrawal.
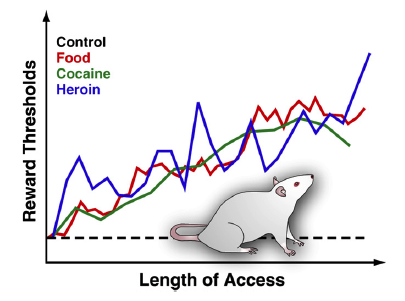
The earlier we start eating hyperpalatable foods, the more likely we are to get hooked on them. This means that good childhood nutrition is very important — and processed foods targeted at children are a major potential health problem.
In related factoids, the longer we’re exposed to innately desirable foods, the more difficult they are to resist. Self-control is a limited resource. So, if you struggle with being near certain foods, get away from them — fast. Get them out of your house, and move yourself away from them. Don’t torture or tempt yourself with physical proximity.
Those who prefer to binge on sweet foods tend to binge more frequently than folks who prefer to binge on fatty or salty foods.
Addicts often have higher levels of dopamine circulating in their brains than non-addicts. It’s not clear whether that’s a cause or consequence of eating.
Binge eating (independent of body weight), rather than weight, is more closely associated with addictive eating patterns. In other words, behaviour predicts addiction better than body size, weight, or fatness.
Some data indicate that compared to women, men are more likely to overeat once they begin, and are more likely to eat more than their body needs.
Philosophical musings
In the U.S., many self-destructive compulsions are considered normal. This means it’s harder to identify problem behaviours as addictions or dependencies. Indeed, if someone were to design a society ideal for food addiction – North America would probably be it.
If we quit eating a certain food – are we addicted to abstaining?
Buddhist teachings have long stated that attachment is the root of all suffering. Could this — along with mindfulness training and learning to “be present” with discomfort — be the key to unlocking addiction?
References
Click here to view the information sources referenced in this article.
Eat, move, and live… better.©
Yep, we know… the health and fitness world can sometimes be a confusing place. But it doesn’t have to be.
Let us help you make sense of it all with this free special report.
In it you’ll learn the best eating, exercise, and lifestyle strategies — unique and personal — for you.



Share