What is dehydration?
When normal conditions exist in the body, various mechanisms preserve fluid and electrolyte balance. If the mechanisms fail due to illness, stress, exercise, climate variations, supplements, foods, or beverages, life threatening imbalances may occur.
Body water in humans varies with age and sex. About 45% to 50% of body weight in females is water. Since males generally have higher amounts of lean mass, body water is around 50% to 60%.
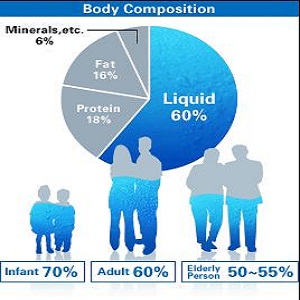
Body water can be found inside of cells, which makes up about 2/3 of total body water, and surrounding cells, which makes up about 1/3 of total body water.
The electrolyte content of these fluids differs greatly. Outside of cells, sodium, chloride, and bicarbonate are the primary electrolytes. Within cells, potassium, magnesium, and phosphate are the primary electrolytes, which is why researchers can use radiolabeled potassium as a marker of lean tissue change.
If the output of fluids exceeds the intake of fluids, an imbalance occurs, and dehydration can develop. The severity of dehydration can be measured by weight loss as a percentage of the normal body weight.
Symptoms of dehydration include:
- thirst
- dry skin
- fatigue and weakness
- increased body temperature
- muscle cramping
- headaches
- nausea
- darker-coloured urine
- dry mucous membranes (mouth, nose, eyes)
Severe dehydration can also include:
- muscle spasms
- vomiting
- dark urine
- vision problems
- loss of consciousness
- kidney and liver failure
Why is dehydration so important?
Body water moves from areas of high solute concentration to areas of low solute concentration (i.e. more dilute) in order to maintain equilibrium in all body compartments.
Water provides the medium for the solubility and passage of nutrients from the blood to the cells and the return of metabolic by-products to the blood. Countless metabolic reactions in the human body rely on water as a medium.
Sensible body water loss (i.e. water loss that we know is occurring) occurs daily in the stool (200 mL), urine (500 to 1500 mL) and sweat. Insensible losses (i.e. those we can’t perceive) occur through the skin (500 mL) and respiratory tract (400 mL). These vary with humidity, environmental temperature and respiratory rate.
The hypothalamus, the renin-angiotensin-aldosterone system, and the kidney are responsible for fluid balance. Anti-diuretic hormone (ADH) and aldosterone are hormones that work with these systems to balance fluid volume. ADH is a water-conserving hormone. Aldosterone stimulates sodium and water retention. The chief stimulus for aldosterone secretion is sodium depletion and associated loss of plasma volume.
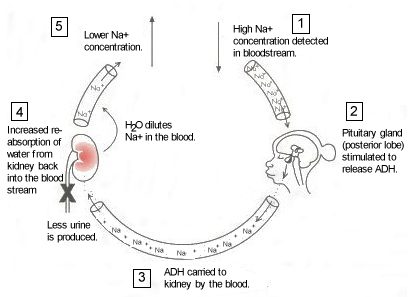
When body water changes, it can have significant effects throughout the body, including athletic performance. Indeed, dehydration of as little as 1% body weight (2 lb for a 200 lb person) is enough to reduce both endurance and strength performance — as well as cognitive performance.
What you should know
During exercise, we need more water. The enhanced metabolic rate of muscle contraction requires a larger delivery of nutrients and oxygen along with faster waste and heat removal from the body.
Exercise is not the only situation that causes alterations in body water. During growth and development, the percentage of body weight that is water and the percentage of water outside and inside of cells do not remain constant. When expressed as a percentage of body weight, body water decreases during gestation and early childhood, attaining adult levels by around 3 years of age.
So where do we get fluids to maintain balance? Well, remember that water intake doesn’t come only from drinking water. It also comes from tea, coffee, non-dairy milks, milks, and water from solid foods. With thirst as a guide, humans are generally well hydrated. There is extreme variability in water needs based on climate and physical activity levels.
Lab screening that qualifies someone for dehydration:
- Osmolality (serum) >295 mOsm/Kg H20
- Sodium (serum) >145 mEq/L
- Albumin higher than normal
- BUN elevated
- BUN:Creatinine ratio >25:1
- Specific gravity >1.031
In the clinical setting, dehydration can be detected by loss of skin elasticity or turgor. If a fold of pinched skin returns to its original shape especially slow (called tenting), then dehydration is suspected (see image below). Conditions such as vomiting, diarrhea or intestinal drainage can also cause fluid imbalances.

However, while dehydration is a concern, overhydration is also something to watch for when planning fluid replacement. Hyponatremia is an electrolyte disorder in which plasma concentrations of sodium fall too low. This is associated with neurological morbidity and mortality. Most cases of hyponatremia are induced by an increase in total body water. This is indicative of impaired free water clearance by the kidneys. Many instances of hyponatremia have occurred because of overdrinking water. For example, as the New England Journal of Medicine reports in a study of Boston Marathoners:
Hyponatremia has emerged as an important cause of race-related death and life-threatening illness among marathon runners… The strongest single predictor of hyponatremia was considerable weight gain during the race, which correlated with excessive fluid intake.
For extra credit
For men, an average of 16 cups of water a day from fluid and non-fluid sources (e.g. fruits and vegetables) is adequate; for women, an average of 11 cups.
Ever wonder why IV fluids are typically given as normal saline? Well, normal saline is 0.9% concentration, similar to that of blood (isotonic).
Loss of plasma volume during prolonged exercise by dehydration diminishes performance in part because of the associate reduction in stroke volume and increases in heart rate known as cardiovascular drift.
ADH production can be affected by alcohol. When we drink alcohol, ADH production is lowered; thus, we urinate more and are thus more easily dehydrated.
Summary and recommendations
Be aware of thirst cues.
If no fluids are going to be given during exercise, you can pre-hydrate with the following regimen:
- 500 ml of fluid on the night before exercise
- 500 ml in the morning
- 500 to 1000 ml, 1 hour before exercise
- 250 to 500ml, 20 minutes before exercise
Consume nutrient dense foods/beverages after exercise to assist in the re-hydrating process.
Those with a history of cramping and “salty sweat” should consider adding salt to foods/beverages after exercising (a quarter to one-half teaspoon).
For every pound of sweat lost during exercise, rehydrate with 2 cups of fluid.
Dark colored urine can be indicative of a low water reserve in the body. So make sure your urine is light-colored and clear.
References
Click here to view the information sources referenced in this article.
Learn more
Want to get in the best shape of your life, and stay that way for good? Check out the following 5-day body transformation courses.
The best part? They're totally free.
To check out the free courses, just click one of the links below.



Share